In this article we’re going to look at one form of technology that is proving to be a positive financial step forward for both the provider organization and the patient with a chronic disease; Remote Patient Monitoring (RPM). We’ll look at its ability to reduce costs on a number of levels:
- By reducing the number of readmissions and unscheduled visits, especially through emergency departments.
- Through a reduction in the need for face-to-face medical professional contact and by improving staff efficiency, all while providing a level of care patients find positive.
- For organizations that have adopted value-based reimbursement models, we’ll show how RPM can help align organizations with the seemingly counter intuitive mandate to provide greater access to care and improve patient outcomes with less financial resources.
Healthcare is in a financial revolution. With annual spend reaching 17.8 percent of GDP, we have approached levels that cause many to conclude the healthcare system is entering a death spiral unless we quickly adopt new, cost-effective technologies and methods of delivering care.
First, a definition...
RPM, often called “telehealth”, takes advantage of Bluetooth enabled medical devices and a computer, tablet or app to deliver critical health indicators to medical staff, all from the comfort of a patient’s home.
At the physician’s choosing, these devices can monitor:
• Pulse, Heart Rate, Blood Pressure and Oxygen Saturation, Blood Glucose Levels, Weight, Cardiac Events, and Help with Medication Management.
Information is forwarded to the physician, clinic or hospital staff via HIPAA-compliant servers. Using preset alerts, when readings fall outside of established parameters staff can then interact and instruct patients quickly and appropriately. This allows the staff and patient to deal with small problems before they become dangerous or life threatening.
Reduced Re-admissions
According to Goldman Sachs, about $1.1 trillion per year is spent in chronic disease management. Of that, it is estimated that 34.5% ($205 billion) is spent in hospital and emergency room visits that could potentially be avoided using RPM. In addition, they report 75% of doctor visits could be handled remotely rather than face-to-face, saving another $100 billion per year. ①
Single Example of RPM Effectiveness:
JH is a 70-year-old female with multiple morbidities of congestive heart failure, primary hypertension, chronic kidney disease, chronic edema and anxiety. Prior to using RPM she had been in the emergency department or been hospitalized an average of once per month for the 18 months prior, mainly for edema and shortness of breath.
Goal: To reduce emergency and hospital visits by 90% in the first 90 days; enhance patient compliance with the plan of care and increase patient understanding of her role in condition management.
Monitoring Provided: Blood pressure, oxygen saturation, pulse, heart rate, weight.
Baseline Data: BP 166/90; Heart Rate 81; Pulse Oxygen Saturation 89%; Weight 282.8; BMI 50.1.
Results:
• Hospital and emergency room visits during the first 90 days dropped to zero, with an average monthly savings of $8,750.
• Through monitoring and subsequent education, the patient’s understanding of how her daily diet affected her condition was greatly improved. Prior to monitoring her daily weight fluctuation could be as much as six pounds.
90 Day Data: BP 137/72; Heart Rate 72; Pulse Oxygen Saturation 96%; Weight 261.1; BMI 46.3.
Broader Studies:
• Sentara Healthcare in Chesapeake, VA, saw a two percent readmission rate for remote monitoring patients versus a 15% rate for the hospital at large. ②
• Partners HealthCare reported a 51% reduction in readmissions for heart failure patients across 1,265 patients enrolled in the RPM program, representing a savings of more then $10.3 million. ③
• CHRISTUS St. Michael Health System in Texarkana, TX, saw the average cost of care drop from $12,937 to $1,231 through the use of RPM in a pilot project tracking 81 year old patients with chronic diseases. ④
• Following a five year study, The Center for Connected Health and the Center for Technology and Aging, both from California, concluded RPM would have an 18.9:1 ROI by year five. ⑤
RPM is fast becoming a valuable tool in driving down readmission and emergency room visit rates. This coincides with the Centers for Medicare & Medicaid Services mandate to reimburse providers on a value-based system with readmit rates being one of their larger determining factors for success and compliance.
The Economics of Reduced Face Time
At a time when there is increased concern over the growing shortage of doctors, patient loads and time allocated toward paperwork and government compliance, any providers throughout the nation are finding RPM to reduce clinic and doctor office visits. This frees up staff for more pressing visits while reducing costs.
➤ In a survey conducted by the American Academy of Family Physicians, the average primary-care doctor saw 19 patients per day with an average encounter of 22 minutes. At approximately the same time, the Physicians Foundation surveyed 13,575 doctors to find that 39.8% see 11 to 20 patients in a day while 26.8% saw 21 to 30 per day. ⑥
Physicians face a growing problem: Patient panel sizes are excessive in the U.S., standing at 2,300 on average, while at the same time we are facing a physician shortage. The Annals of Family Medicine has concluded that it would take doctors 21.7 hours per day to provide all of the recommended care, for acute, chronic and preventative visits, if the number of patients should swell to 2,500 members per panel.
But here is what is interesting:
➤ Authors of the same article conducted an analysis of patient numbers, average time at visit and panel sizes. They then studied three assumptions which impacted panel size when a certain amount of medical professional interaction could be shifted to non-physician team members. (They also took into account the variances in needed time of interaction for preventative and chronic patient visits and repeat visits.)
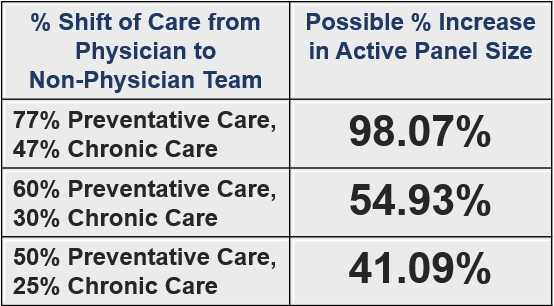
Modeling assumptions on a shift from face-to-face physician interaction to some degree of non-physician team member interaction, the authors concluded that providing the recommended amount of preventative and chronic care could be achieved with the current physician workforce. ⑦
(Note that the “recommended amount of preventative and chronic care” translated to 983 patients actively seeking and receiving care out of an average panel size of 2,500.)
Through the use of RPM this seems to already be a reality, which is good news for physicians and patients alike.
Examples:
• Partners Healthcare monitored the number of patients using RPM to non-physician team members in two groups; cardiac patients and patients with other acute illnesses. For cardiac patients, four nurses could monitor 250 patients on a daily basis (62.5 patients/nurse). For other acute patients, 80-100 patients per day per nurse was the norm.
• Essentia Health’s experience was approximately the same. There, through the use of RPM, 14 registered nurses and fourteen nurse practitioners monitor 2,300 patients per day, or about 82.14 patients per non-physician team member. They also saw readmission rates drop while patients actually felt more connected to their physician, even though they saw the physician less.
It appears that the assumptions made by RPM proponents have validity. With the squeeze physicians are feeling due to increased case loads, RPM can shift some of the burden to non-physician staff. This effectively increases the case load for physicians without increasing their daily hours, shortens waiting times before the next appointment for those that must be seen by a physician and more efficiently makes use of non-physician staff members by the sheer number of patients they can monitor.
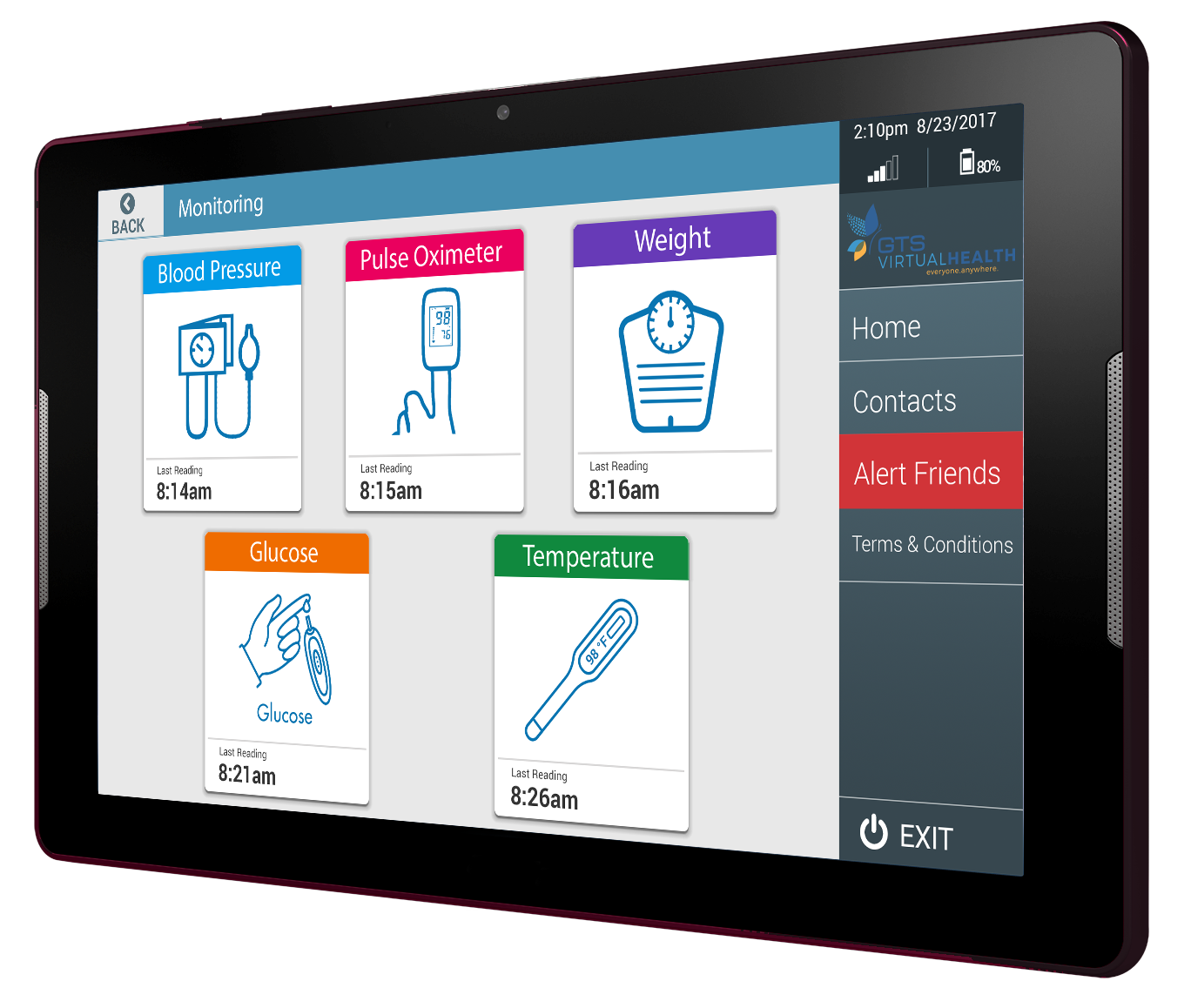
1 Nurse Monitoring ~83 Patients Daily
But what do patients say?
When the Government Accountability Office ⑨ surveyed patient association/advocacy groups, respondents gave RPM high praise in five areas (with a possible score of “10” in each). Results were as follows:
✓ Improving or Maintaining Quality of Care - 10
✓ Alleviation of Provider Shortages/Scheduling - 10
✓ Convenience for the Patient/Family - 10
✓ Coverage of Services - 8
✓ Cost Reduction - 8
Using RPM, patients often feel they are more connected to their health team, learn more about their diagnosis and their role in remaining on a healthier track and enjoy not having to arrange numerous visits or transportation. They also often cite feeling less anxious about their condition because they feel someone is looking over their shoulder.
Remote Patient Monitoring and ACOs
One of the biggest challenges facing health care organizations is the switch from fee-forservice methods of payment to value-based reimbursement brought on by the Medicare Shared Savings Program (MSSP) from The Centers for Medicare and Medicaid Services (CMS). Patients and their health care providers most effected, the High Need High Cost patient (due to chronic conditions), make up only five percent of the US population but account for 49% of health care expenses.
This translates to nearly half of the health care organization’s budget falling under the three-point goal of CMS:
• Enhancing patient outcomes,
• Enabling greater patient access to health care,
• While cutting costs.
The target to achieving reduced costs is through fewer readmissions and emergency department visits by patients past the initial diagnosis and treatment of a condition.
It’s beyond the scope of this article to dive into the mandates of MSSP. In short, the health care organization is being told they must provide more with less financial resources. If the Accountable Care Organization (ACO) meets its target goal of achieving the three above CMS mandates, it will share in the pool of savings CMS enjoyed through the ACO’s costreducing practices. We’ve already seen how RPM can reduce the number of readmissions and emergency department visits from this patient population. We’ve also looked at how a physician group can cope with shrinking budgets while providing greater access to continuous care through RPM. But how is the ACO as an organization integrating RPM to achieve these goals?
Here is a little background: In 2013 there were 220 ACOs which provided care to 3.7 million Medicare users. By 2016 those numbers had grown to 432 and 7.8 million respectively. During this time, the metrics CMS wants to see have improved, but many health care organizations are realizing it can take several years to achieve minimum requirements. It took many three years to go from a CMS score of 63.77 to 73.15.⑩
In an effort to speed up compliance and gain a bigger share of the yearly “bonuses”, 79% of ACOs surveyed say they already have or are looking into the use of RPM. The obvious benefit is RPM’s ability to provide greater patient access to care while reducing readmissions and emergency department visits. But those already using RPM cite several other benefits as well:
- Access to increased frequency of patient data.
- Support for an increased level of accuracy for clinical monitoring readings.
- The ability to interpret the larger data sets for overall decision making in the health care organization.
From the patient to the immediate physician and on to the larger organization, RPM can speed up the success matrix CMS is looking for.
For the ACO (and eventually all health care organizations that wish to remain treating Medicare and Medicaid patients) three things are evident:
- Reimbursement by CMS will be, or already is, reduced, and the only way to make up some of the lost revenue will be by proving to CMS that the organization can meet government mandates.
- The financial stakes are large and growing, with MSSP payments eaching $645 million in 2015, nearly double the amount from the year before - and we are still not in full implementation of the MSSP program.
- RPM has proven itself effective in helping to achieve many of the requirements laid out by CMS if the ACO ever hopes to receive its share of the savings “pool”. The CMS mandate is also clear: Cut costs and drive positive outcomes or we’ll do it for you.
Summary
We’ve looked at three areas of financial savings that RPM can provide:
• By reducing the number of readmissions and emergency department visits while providing the patient immediate access to his or her health care team, giving him or her increased pre-event instruction and intervention.
• By shifting the growing case burden on physicians to non-physician staff who can remotely monitor vastly larger numbers of patients; in so doing, staff efficiency is increased while the physician can oversee a bigger case load within the allowed timeframe.
• By aligning organizations with the seemingly counter-intuitive mandate to provide greater access to care and improve patient outcomes with less financial resources, while giving decision makers more data for informed choices.
We do not pretend to believe RPM can solve 100% of the issues of repeated emergency department visits or readmits, growing panels or the challenge of MSSP. But it has proven itself to be a technical solution to a large part of all of these issues, and patients surveyed seem to be ready for the convenience and connection RPM provides with health care providers.

